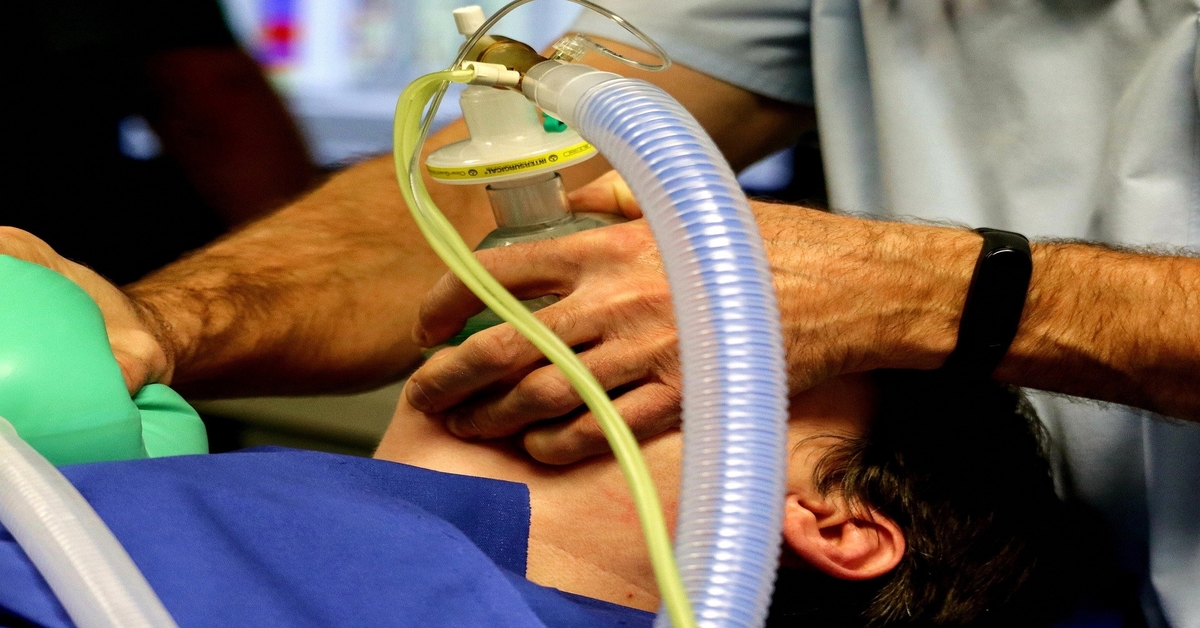
2 Reasons Heart Attack can take you to a Ventilator
-
- Dr. Junaid Arshad
- December 29, 2021
- 0 comments
Introduction
Heart Attacks can have a variety of presentations, ranging from silent MI that remains undetected to sudden cardiac death that usually occurs in a prehospital setting.
A handful of patients develop such complications with a heart attack that they require mechanical ventilation & have a very high mortality rate.
This article explains in detail the 2 reasons for mechanical ventilation in a patient suffering from a heart attack, & also the survival rate in such patients.
Heart Failure
Heart failure in a patient with a heart attack or acute MI can necessitate the need for mechanical ventilation for several reasons. This holds true particularly for advanced heart failure with cardiogenic shock.
Cardiogenic shock is defined as the inability of the heart to effectively pump the blood resulting in decreased perfusion (blood supply) to the organs. It is characterized by a persistently low blood pressure of systolic <80 to 90 mmHg or a mean arterial pressure 30 mmHg lower than baseline.
Fortunately, the incidence of advanced heart failure with cardiogenic shock after acute MI is on a decreasing trend since the 1970s.
The reason for this decreasing trend is probably an increased utilization of early coronary reperfusion therapies like PCI & thrombolysis that help salvage the myocardium and reduce the incidence of mechanical complications & hence improving the outcomes. [1]
Reasons for the requirement of Ventilator for heart failure after a heart attack
These include the following:
Protection of Airway
Patients with advanced heart failure may develop a decreased conscious level which itself is an indication for mechanical ventilation as these patients are at increased risk of airway obstruction and aspiration.
The most common reason for airway obstruction is the fallback of the tongue.
Endotracheal intubation & mechanical ventilation help prevent this life-threatening complication.
Treatment of respiratory failure
Patients with heart failure develop respiratory failure as well because the left side of the heart is unable to effectively pump the blood in forward direction.
This leads to accumulation & back pooling of blood within the blood vessels of the lungs & hence a condition called pulmonary edema.
Lungs are unable to carry out their proper function resulting in a decreased oxygenation of blood.
Mechanical ventilation helps with the oxygenation process and is continued till the time pulmonary edema settles and lung the function returns to normal.
Treatment of metabolic acidosis
Decreased tissue perfusion & decreased oxygenation cause increased production of lactate & hence cause metabolic acidosis.
Patients with heart failure suffer both decreased tissue perfusion as a result of cardiogenic shock and decreased oxygenation as a result of respiratory failure & pulmonary edema.
Metabolic acidosis further adds to adverse effects on the heart, lungs, and also the brain & is associated with worse outcomes.
The use of mechanical ventilation improves the oxygenation of blood thus increasing arterial pH and helping correct metabolic acidosis.
Prognosis
Unfortunately, the prognosis of patients who develop heart failure and shock requiring mechanical ventilation after a heart attack isn’t good & in-hospital mortality reaches over 50%. The severity of shock & hemodynamic compromise determines the outcomes. Another factor that contributes to a higher mortality rate is the presence of multi-organ dysfunction which is present in almost 32% of these patients.
The patients who survive this acute condition and undergo timely revascularization have an improved survival rate & quality of life in the long term.
The presence of the following factors is associated with a worse prognosis.
- Old Age
- Clinical signs of decreased organ perfusion which include decreased urine output, cold clammy extremities, or biochemiacl evidence such as raised lactate levels, derrange renal functions, raised ALT, & low sodium levels. [2]
- History of stroke.
- Reduced mean arterial pressure despite of inotropic support.
- Presence of NSTEMI as opposed to STEMI.
Ventricular Arrhythmias
Ventricular tachyarrhythmias like VT & VF are not very uncommon with a heart attack and those who survive these dreadful conditions usually require mechanical ventilation.
Both VT & VF can lead to sudden cardiac death (SCD) if not treated immediately.
Although the incidence of SCD after a heart attack has decreased with the advancement in revascularization strategies like PCI and fibrinolysis, still ventricular arrhythmias remain its common cause
Statistics have shown that up to 6% of the patients with heart attack develop VT/VF within the first 48 hours.
Ventricular Tachycardia (VT)
VT or Ventricular tachycardia refers to a condition when the ventricles of the heart start beating fast, at more than 100 b.p.m. & the heart rhythm that normally originates from the atria (the two upper chambers of the heart) starts to originate from the ventricles (the two lower chambers of the heart) instead.
Patients with VT may or may not undergo a hemodynamic compromise.
Hemodynamic compromise means that the heart is unable to generate enough blood pressure to maintain blood supply to vital organs including the brain & kidneys.
The patients who get hemodynamically compromised require mechanical ventilation after they are reverted back to a normal rhythm. These patients have a very poor prognosis and in-hospital mortality is very high, as much as 6 times more than those who do not develop VT and do not require a ventilator.
Those who survive the ventricular arrhythmias and get weaned off the ventilator have a good prognosis in long term.
Whereas those who develop hemodynamically stable VT, may not require mechanical ventilation & have a good prognosis overall.
Ventricular Fibrillation (VF)
On the other hand, Ventricular fibrillation (VF) is an even more dangerous condition in which ventricles undergo twitching movements instead of proper contractions, this results in hemodynamic compromise and sudden cessation of blood supply to all the organs including the brain.
VF s the underlying mechanism in most cases of SCD & if not immediately treated is always fatal & those who are rescued always require a ventilator.
It usually occurs within the first 48-72 hours of a heart attack.
Factors that increase the risk of VF in patients with a heart attack are as under.
- Massive heart attack involving larger area of heart muscle
- ST elevation typye of heart attack (STEMI)
- Electrolyted abnormalities like low potassium
- Low blood pressure
- Male gender
- Hisotry of smoking
- Inferior wall heart attack
Patient survival in patients with VF on mechanical ventilation is similar to that mentioned previously for VT. Mortality is high and most of the patients die within the first 30 days. Those who recover have better long-term survival.
Q & A
Can a Ventilator cause a heart attack?
A patient on a ventilator is in a critical state and usually develops multiorgan dysfunction. All the organs including the heart are under great stress. Patients may suffer a Type-2 MI which is due to the increased workload on the heart where the heart requires more energy but the body is unable to meet the energy demands.
Is it common to be put on a ventilator after a heart attack?
In the era of Primary PCI and thrombolysis, the number of patients who require a ventilator after a heart attack has decreased & is not very common. However, the exact number is difficult to mention as the data is lacking and there are variations amongst the results of different studies.
How long can you be on a ventilator after a heart attack?
The time a patient needs to be on a ventilator varies from patient to patient. Some patients may need it just for a day or two and others might stay on it for weeks. This is to be decided by the team of doctors including a cardiologist & an ICU specialist. It depends upon multiple factors like the functioning of each organ system including the lungs, heart, brain, & kidneys.
Why do you need a ventilator after a heart attack?
A patient needs a ventilator after a heart attack as a result of any complication that compromises heart function to such an extent that it cannot maintain the blood supply of individual organs. Heart Failure & ventricular arrhythmias like VT & VF are the main causes. Patients’ conscious level deteriorates as a result of decreased brain perfusion & lungs get filled with fluid and the respiratory system fails. Mechanical ventilation may help save the patient although mortality is quite high.
Latest Posts
-

-

Can You Use Expired Glucometer Test Strips? What You Need to Know
December 29, 2021 -
-

Categories
- Cardiology 32 Posts
- Diabetes 4 Posts
- Drugs 1 Post
- Infectious Diseases 2 Posts
- Sexual Health 3 Posts